City Footcare NYC
Surgery & Medicine of the Foot & Ankle
End Foot Pain Now
Welcome to CityFootcare.com!
We are group of 4 podiatrists located in Midtown Manhattan.
We offer the best care in Podiatric Medicine and Surgery in NYC.
The doctors at City Footcare NYC are the most compassionate and skilled foot doctors in the New York City Metro area and the country. Our office is conveniently located in Midtown Manhattan near Grand Central Station. We take great pride in providing excellent medical care along with great bedside manner and take the extra time to explain your problems and the treatment options in detail.
At City Footcare NYC we treat all problems related to the foot and ankle. We use state of the art diagnostic and therapeutic equipment. When your problem requires surgery, you can rest assured that you are in the hands of a competent and highly trained surgeon. Most of our doctors perform surgery and Dr. Sergi specifically only does foot surgery and not general podiatry (ask about individual providers).
Dr. Sergi has been called the best foot surgeon in NYC and the best bunion surgeon in NYC. The doctor performs all foot and ankle surgery including traditional open surgery, minimally invasive surgery, laser surgery, radio frequency surgery and extra-corporeal shock wave therapy. He is surgery center affiliated.
To resolve all of your foot and ankle problems, simply look around this site and make an appointment with the doctors at City Footcare NYC today. Your feet will be glad you did!
End foot pain now!
You don’t have to spend another day suffering from foot pain! Let the City Footcare NYC doctors help you to END FOOT PAIN NOW! Call today to schedule an appointment and take the first step toward many more comfortable steps in the future.
Compassionate and caring
- Full treatment Facility
- Latest technology
- Most Insurances Accepted
- Convenient Location
Office Hours
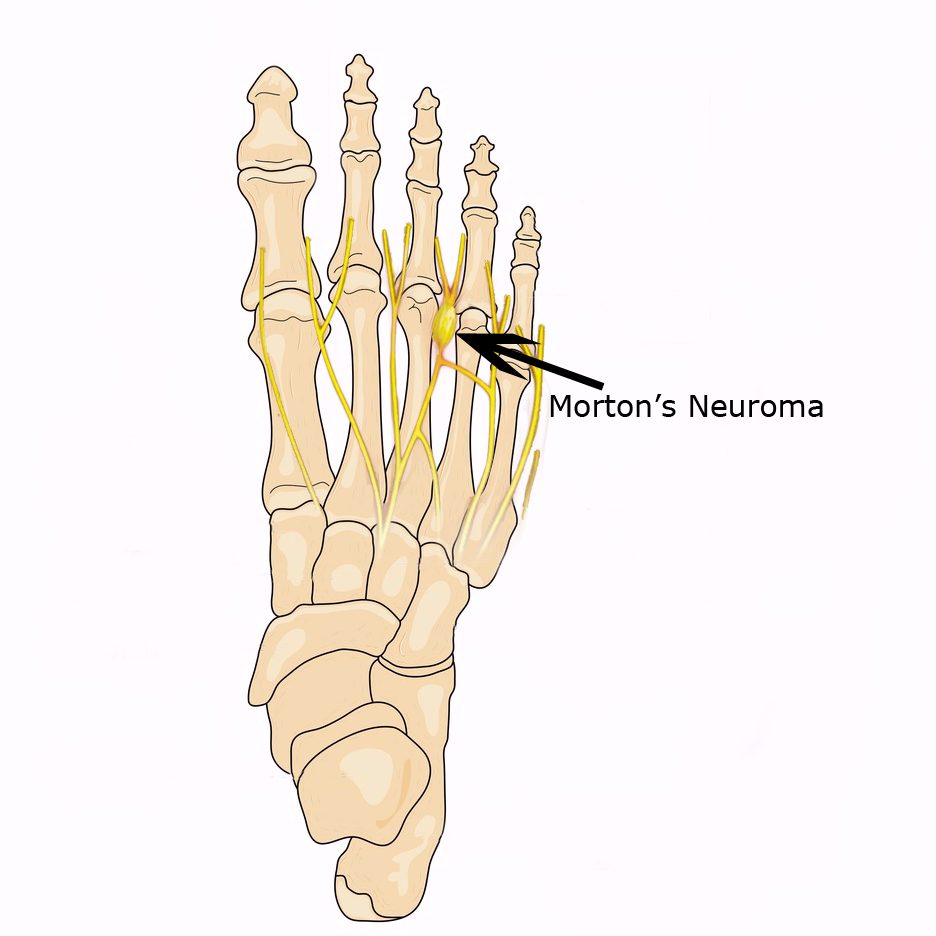
A fun cartoon to explain bunion surgery!
Experts in Foot Surgery
When your problem requires surgery, you can rest assured that you are in the hands of a competent and highly trained surgeon.
Dr. Sergi and the City Footcare NYC Doctors have been called the best foot surgeons in NYC and the best bunion surgeons in NYC.
The doctors perform all foot and ankle surgery including traditional open surgery, minimally invasive surgery, laser surgery, radio frequency surgery and extra-corporeal shock wave therapy.
Dr. Sergi and the City Footcare NYC Doctors are experts in all aspects of foot surgery. They are very detail oriented from start to finish.
A good surgical outcome starts prior to entering the operating room. After expertly diagnosing patients’ conditions, they plan out the procedures with great skill.
In the operating room they are skillful and precise. They also take into consideration aesthetics with incision planning and plastic surgery type suturing techniques.
They are surgery center credentialled & affiliated.
Please see the medical DISCLAIMER on the 'about this blog page'.
Our Google Reviews.
"Dr. Sergi is knowledgeable and has good experience of fixing foot problem. He explains clearly the operation procedure and post-op care. He has confidence in his operation. He is also considerate of patient and has a warm heart to wrap surgical foot with bright color bandage. This is my third week since my surgery and I feel good to see my foot is free of bunion. I don't have pain from bunion or surgery. I am very lucky my foot has been fixed by a successful doctor who is expert in foot care operation."
"The best decision I could of done was to do my foot surgery with Dr. Emanuel Sergi.
He is the best, very caring and very professional.
I went to him for a second opinion and I am so glad I decided to do my foot surgery with him.
All I had to do was follow his instructions and my foot feels good and it’s healing very good also.
Thank you Dr. Sergi."